Think you are suffering from non-celiac gluten sensitivity? This article attempts to sort through the hype, the myths and misinformation, and get to the truth about gluten-free diets, if they are right for you and the possible causes of symptoms that are often attributed to gluten, so you can make informed choices about your health and diet.
Let’s look at exactly what the research says and the legitimacy of non-celiac gluten sensitivity, why it is being called into question and if there could be other underlying causes of symptoms attributed to gluten-sensitivity.
Though the percentage of people diagnosed with celiac has remained relatively unchanged at approximately 1% of the general population, the number of people switching over to a gluten-free diet has sky rocketed in recent years. So what’s going on?
What is gluten and where do you find it?
In Latin, gluten means “glue” and that’s exactly what it is: two proteins, gliadin and glutenin, stuck together. Gluten is used as a binding ingredient and it’s what gives some foods its chewy, elastic properties. It’s found in wheat, barley and rye, which means it is in a myriad of products, from the usual suspects, like bread, bagels, pastries and pasta to those that are not nearly so obvious, things like hard candies, jelly beans, cold cuts, licorice, gravy, whiskey, flavoured potato chips, and canned soups and sauces, hydrolyzed protein, plant protein, vegetable protein, stabilizers and emulsifiers.
I know what you might be thinking – you probably shouldn’t be eating those ‘unusual suspects anyway as they are processed and not very good for you, but here is a surprising list of foods more likely to make it into a health-conscious diet that also contain gluten: soy sauce, couscous, oatmeal, spelt, barley, kamut, dry roasted nuts, California rolls, meat substitutes, ground spices (flour is often added to prevent caking to extend shelf life), some dairy substitutes, some salad dressings, miso, soba noodles.
Celiac Disease vs. Gluten Sensitivity & Food Intolerance vs. Food Allergy
Celiac disease is more than a sensitivity. Approximately 1% of the population has been diagnosed with celiac disease, which is a serious auto-immune disease that occurs in genetically predisposed people where the ingestion of gluten leads to damage in the small intestine. In people with the condition, eating the protein prompts the immune system to attack the small intestine, leading to digestive complaints, such as diarrhea, bloating and weight loss. The rejection of gluten can affect the absorption rate of many other nutrients that are key to our wellbeing, including iron, calcium, vitamins A, D, E, K, and folate [ref.1].
Non-celiac gluten sensitivity on the other hand, is an undiagnosed and largely unrecognized condition by the medical community, the definition of which is not succinctly defined anywhere, except to say that it describes people who experience symptoms similar to celiac disease when they eat gluten, without the intestinal damage.
General food intolerance (also sometimes called a sensitivity), as explained by the American Academy of Allergy, Asthma, and Immunology, takes place in the digestive system. It happens when you’re not easily able to break down the food you eat. This can be caused by enzyme deficiencies, sensitivity to a food, or a reaction to naturally-occurring food chemicals. Typically, people with an intolerance or sensitivity can eat these foods in small amounts without experiencing problems.[ref.2]
Food Allergy is an immune system reaction that occurs soon after eating a certain food. Even a tiny amount of the allergy-causing food can trigger signs and symptoms such as digestive problems, hives or swollen airways. In some people, a food allergy can cause severe symptoms or even a life-threatening reaction known as anaphylaxis. [ref.3]
Home Food Sensitivity Test Kits
Home food sensitivity test kits started to become popular in the last few years, despite being completely unregulated and never having had any credible science to substantiate them. They may be a significant factor in the rise of gluten sensitivity self-diagnoses as all invariably almost always test positive for gluten, dairy and soy. Here’s why…
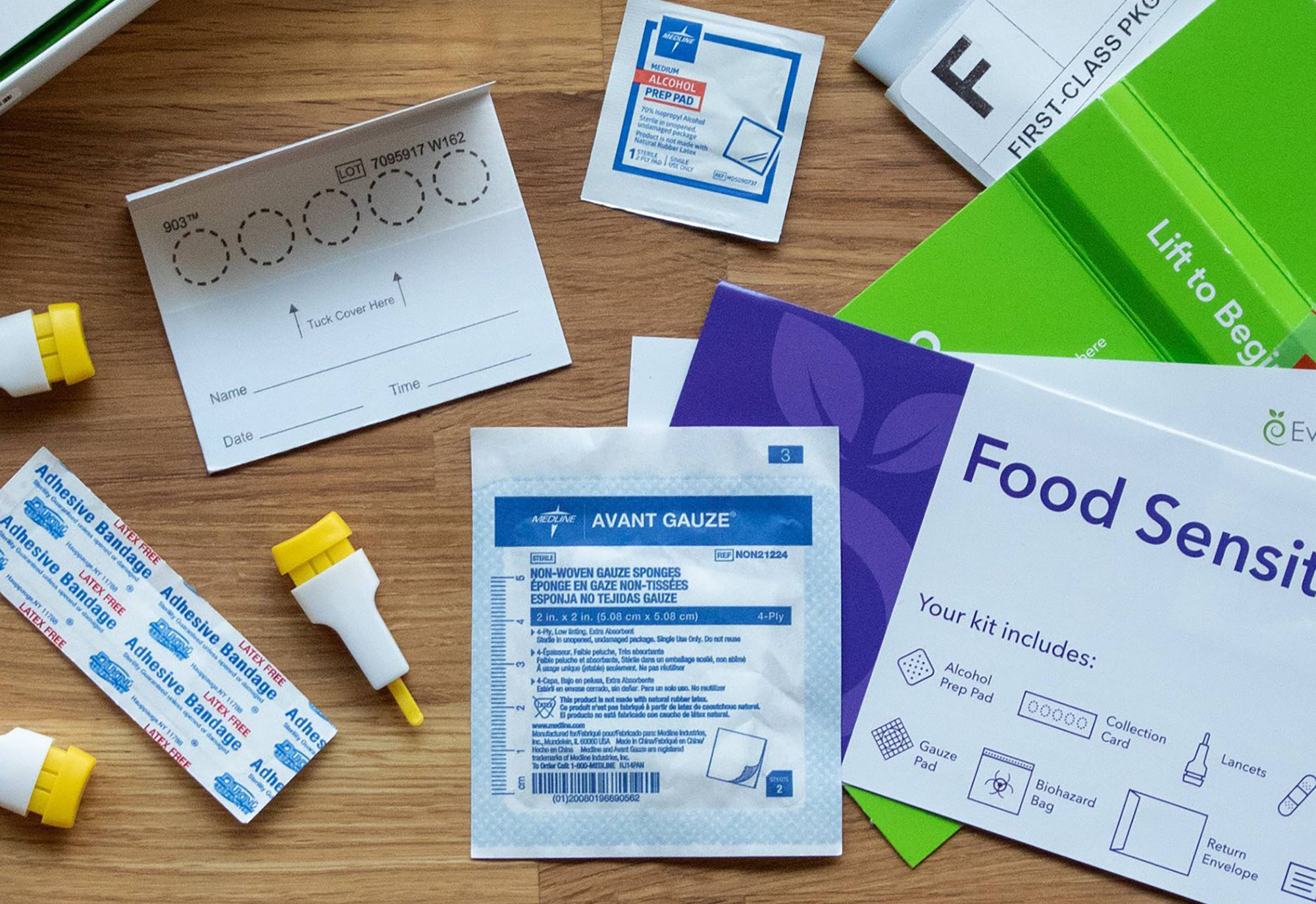
Whereas food allergy blood tests measure Immunoglobulin E (IgE), an antibody that attacks foreign proteins that produces an allergic response, many food sensitivity test kits measure Immunoglobulin G (IgG), antibodies which stem from the body’s normal immune response to exposure to many substances, including food. High levels don’t indicate a problem; they simply point to foods a person recently has eaten.
In a 2018 article [ref.4] in the journal Allergy and Clinical Immunology: In Practice explains, “the production of IgG antibodies to foods is a normal immunologic phenomenon. IgG antibodies to foods are found in virtually all healthy individuals.”
The article goes on to state that European Academy of Allergy and Clinical Immunology, the American Academy of Allergy, Asthma, and Immunology, and the Canadian Society of Allergy and Clinical Immunology have all issued papers, statements, and endorsements that positive test results for food-specific IgG are to be expected in healthy adults and children, and not an accurate measurement of food sensitivity. [ref.5, ref.6, ref.7]
In short, most of the home food sensitivity test kits are not an accurate way to diagnose any type of food sensitivity.
Let’s look at the research into Gluten Sensitivity
Several studies have suggested that most people who believe they’re gluten sensitive don’t react to gluten at all. Studies done with those suffering from Irritable Bowel syndrome (which would make them the most likely candidates to experience the gastro intestinal side effects of gluten) and self-diagnosed gluten sensitivity, when introduced to isolated gluten, had no dietary effect on the participants (ref.8)
So what – it’s all in my head?
If you are experiencing abdominal distress, dizziness, fatigue and/or bowel issues or a general feeling of unwellness from what you think may be attributed to gluten, there is research to support that you are not crazy, don’t worry.
Clinical trials on celiac biomarkers have found that some people report gastrointestinal improvements on a gluten free diet even when they don’t carry the celiac biomarkers [ref.9, ref.10, and ref.11). Other studies (ref.12, href.13,and ref.14) have found people with self-diagnosed Non Celiac Gluten Sensitivity had some abnormalities of their antibodies that hint towards some sort of systemic immune activation that is different from celiac disease.
All of these studies offer some support for Non Celiac Gluten Sensitivity but they come with serious methodological limitations. Most notably, they don’t isolate gluten from other components that may also come part and parcel in a gluten free diet. In other words, is it actually a sensitivity to gluten specifically, or is it another protein in wheat, a sugar in grains, an additive, or something else?
FODMAPS – what they are and why you need to know
FODMAPs (Fermentable, Oligo-, Di-, Mono-saccharides And Polyols). are short chain carbohydrates (oligosaccharides), disaccharides, monosaccharides and related alcohols that are poorly absorbed in the small intestine. Growing evidence suggests the involvement of FODMAPs, a category of carbs and fiber that may cause digestive discomfort, are likely the main culprit in the misdiagnosis of gluten intolerance.
Studies [ref.15] have been conducted to investigate the specific effects of gluten after dietary reduction of FODMAPs and it was concluded that these individuals’ supposed gluten sensitivity was more likely a sensitivity to FODMAPs.
Another study which supported these findings revealed that people with self-reported gluten sensitivity didn’t react to gluten but to fructans, a category of FODMAPs in wheat (ref.16].
While FODMAPs are currently believed to be the main reason for self-reported gluten sensitivity, and it’s been agreed that gluten sensitivity is a bit of a misnomer and should be more aptly named a wheat sensitivity [ref.17], gluten hasn’t been completely ruled out.
The rise of the Gluten-free Diet
Though the percentage of people diagnosed with celiac has remained relatively unchanged at approximately 1% of the general population, the number of people switching over to a gluten-free diet has sky rocketed in recent years. So what’s going on?
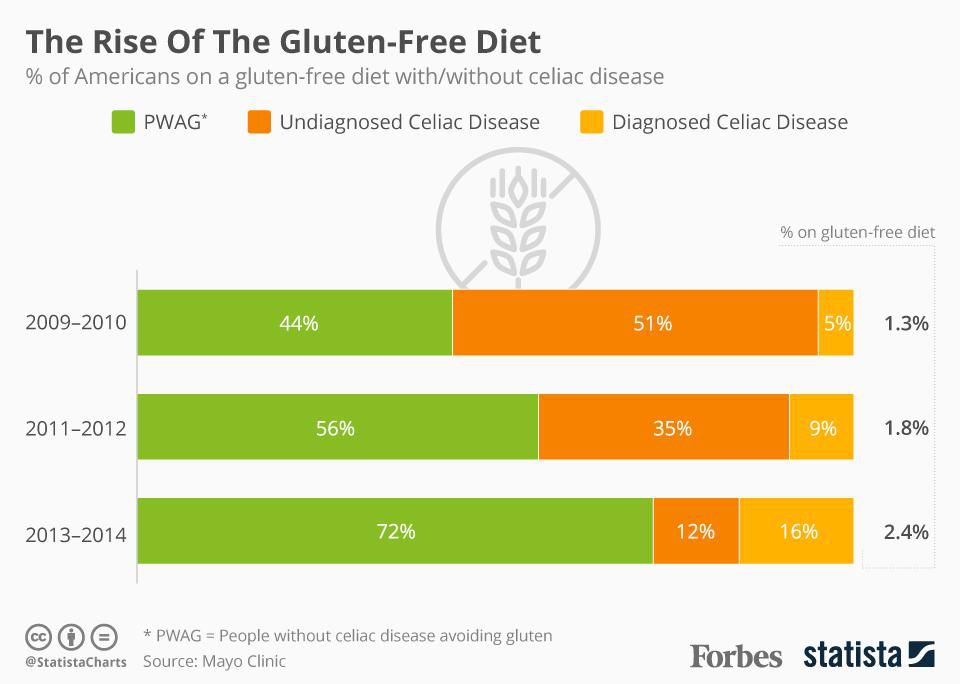
To find out how many people are truly gluten-sensitive, researchers from the University of L’Aquila in Italy enrolled 392 patients who believed they had gluten sensitivity into a controlled clinical trial. Results: Of the 392 patients, 6.63 percent tested positive for celiac disease, and two individuals (.51 percent) for wheat allergy. Some 27 patients (6.88 percent) were found to suffer from some form of non-celiac gluten/wheat sensitivity. Based on this, 86 percent of those who believe they’re sensitive to gluten can tolerate it without negative health consequences. [ref.17]
That doesn’t explain why an estimated 30 percent of shoppers are choosing gluten-free options, and 41 percent of U.S. adults believe gluten-free foods are beneficial for everyone [ref.18].
Some of the reasons that Gluten Free Diets are on the Rise
Celiac disease and wheat allergies not being properly diagnosed
Though celiac disease is estimated as afflicting approximately 1% of the population, A 2012 Mayo Clinic survey suggests that celiac disease may be underdiagnosed. Up to 1.4 of the 1.8 million Americans thought to have celiac disease may not know they do [ref.19]. As the study at the University of L’Aquila in Italy found – of the 392 study participants that thought themselves to be gluten-sensitive, 6.63% of those participants actually tested positive for Celiac Disease, a far larger percentage than the 1% of the population estimated to have Celiac Disease. Behind the misdiagnosis of Celiac, an allergy to wheat is one of the other contributors to symptoms mis-associated to gluten sensitivity.
Bad Press
After being confined to health-food stores for years, gluten-free foods now show up everywhere. Supermarket aisles abound with products proudly labeled “Gluten free,” and many restaurants now offer gluten-free options. Fueled in part by recent bestselling books, and the television talk shows and celebrity endorsements that accompany them that warn of the evils of gluten in our diets, a significant proportion of our population is rapidly changing its eating habits. The gluten-free trend—and the accompanying multibillion-dollar industry it has created—stems from the spreading the unsubstantiated beliefs that eating foods containing gluten may not only result in weight gain and obesity, but can also lead to a laundry list of ailments ranging from alzheimers and anxiety to arthritis and autism, just to name a few.
The Placebo & Nocebo effect
The placebo effect will have people experience the benefits of drugs that are really just sugar pills [ref.20]. As Muhammad Ali regularly professed “I am the greatest”, said: “if you say something enough, people will start to believe it.” Afterall, we’ve spent the last 5 + years reading that gluten is the devil, so it’s pretty hard not to absorb and internalize some of that information. So if you everyone around you and scores of celebrities are professing to feel better on a gluten free diet, it may be that you don’t actually suffer from a sensitivity to gluten, but you still might feel better because you expect to.
For some people, something called the “nocebo effect” may be at work. It’s like the flip side of the placebo effect, whereby If you believe something – be it a pill or a protein (i.e gluten) – will cause you physical harm, it can, even if it’s actually innocuous… which would explain why many of those who reintroduce gluten into their diet after having gone gluten-free are convinced they feel worse.
The Belief That a Gluten Free Diet will Aid in Weight Loss
This is a myth as most gluten-free products are not only higher in calories, but in fat, sugar and sodium as well, not to mention having less fibre and protein than the same products that contain gluten.
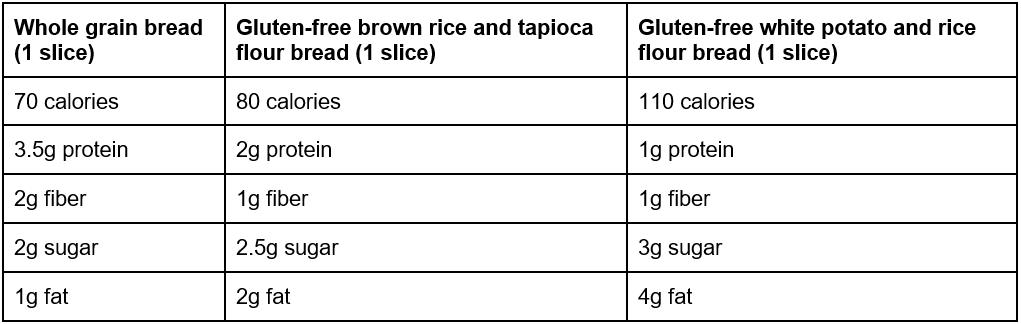
Nutrient data obtained from the USDA Food Composition Database
Is a gluten free diet for you?
Carol Johnston, professor and associate director of the Nutrition Program in the College of Health Solutions says: “There is no clear evidence that avoiding gluten offers any health benefits for the majority of the population.” This is a sentiment that is echoed by most health professionals, who further go on to warn about the harmful side effects of a gluten-free diet if you have not been diagnosed to have celiac disease, a wheat allergy or sensitivity.
Gluten is important for the absorption of iron, calcium and fiber, vitamins A, D, E, K, and folate [ref.21]. Taking gluten out of your diet may lead to nutritional deficiencies. Studies have also shown groups with the highest intakes of whole grains including wheat (2-3 servings daily) compared with groups eating the lowest amounts (less than 2 servings daily) were found to have significantly lower rates of heart disease and stroke, and development of type 2 diabetes.
Grains are also one of the best sources of beneficial prebiotics. Eliminating those beneficial prebiotics in grains may change the healthy gut microflora and increase the risk for chronic disease. [ref.23] Arabinoxylan oligosaccharide is a prebiotic carbohydrate derived from wheat bran that has been shown to stimulate the activity of bifidobacteria in the colon. These bacteria are normally found in a healthy human gut. Changes in their amount or activity have been associated with gastrointestinal diseases including inflammatory bowel disease, colorectal cancer, and irritable bowel syndrome. [ref.24]
With the rise of an awareness of promoting ‘gut health’, it is likely that gluten-free diets for those without a diagnosis of celiac, a wheat allergy or sensitivity, is a diet trend on its way out.
Summary
Like celiac disease and wheat allergies, a wheat sensitivity is not as prevalent as many believe. What’s more, eating a gluten-free diet isn’t necessarily healthier, nor is it recommended for weight loss. It’s important to find out if you’ve been sucked into a trendy fad or it’s a legitimate health strategy for you.
If you find yourself suspecting you have a gluten sensitivity, the thing to do is to first get yourself tested by a doctor for a wheat allergy and for celiac disease. If both come back negative, keep a detailed food and symptom log for two full weeks. Write down the time of everything you eat with details – down to the brand when appropriate – and the time of any adverse symptoms you may experience. Bring this information to a reputable registered dietitian – ideally one who specializes in food allergy or gastrointestinal issues and doesn’t sell any supplements, so that he/she can help you identify the common threads among likely trigger foods or meals. This exercise will most likely yield a sane, manageable diet trial that you can undertake toward identifying the precise nature of your symptoms.





Leave A Comment